Among coronavirus patients, rural older Americans have worst obstacles
Roughly 69% of the United States' rural population is over the age of 65
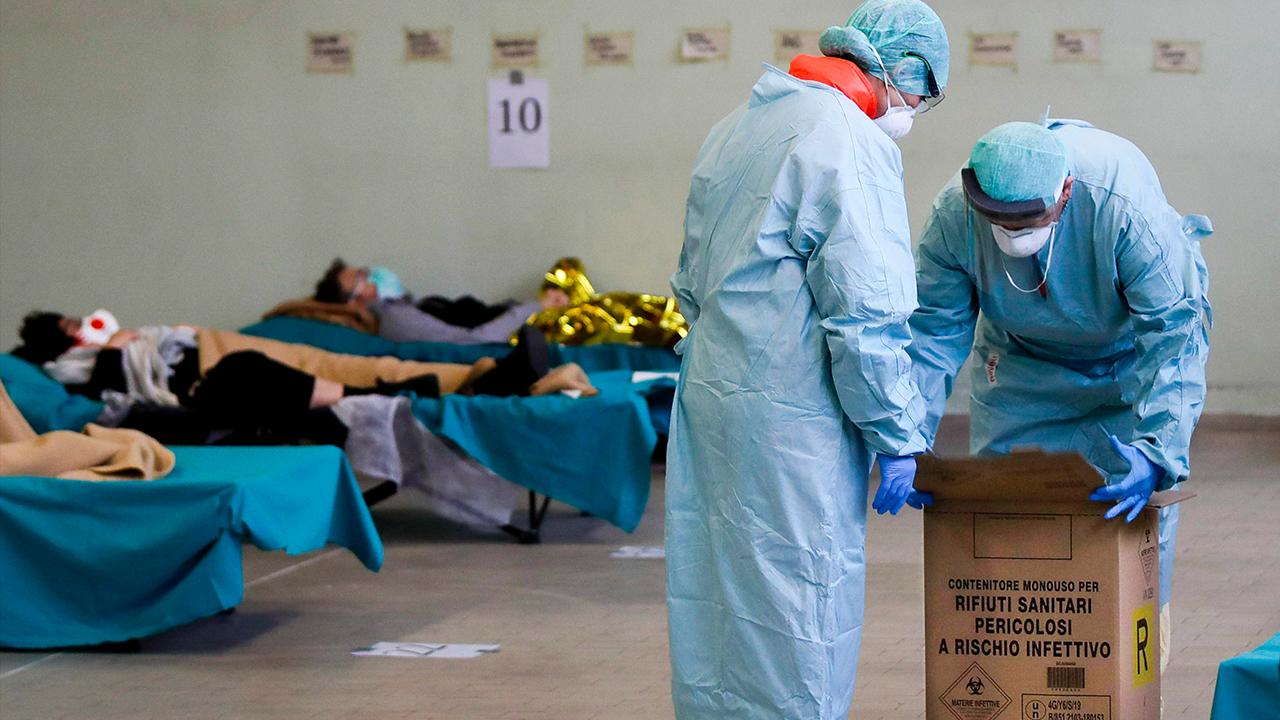
As everyone goes into social isolation to distance themselves from other Americans in an effort to "flatten the curve," citizens who are the most vulnerable and likely to face the worst circumstances if they contract COVID-19 are rural residents facing major downsizing to hospital care.
Rural areas face many obstacles should they encounter a coronavirus outbreak. Hospital drives could be 60 to 90 miles away to the closest major city, which puts the most at-risk residents such as older, poorer and sicker patients at a disadvantage.
Harrison County, Kentucky, which has a population of 19,000, saw the state's first cases of coronavirus, but it’s almost an hour’s drive from an urban center, Lexington.
CORONAVIRUS OUTBREAK INCREASES DEMAND FOR MEALS ON WHEELS
The people most at risk of contracting COVID-19 and succumbing to the aggressive nature of the virus are patients who are over the age of 60 and/or have preexisting health conditions.
Roughly 69 percent of the United States' rural population is over the age of 65, compared to 35 percent of the non-rural population, according to a January research study from the Chartis Group, a health care consulting firm.
“If you have no place to go or if you have to drive an additional hour or two to get somewhere, people just don’t go,” said Doug Farquhar, program director for environmental health at the National Conference of State Legislatures. “This virus doesn’t seem to be avoiding rural areas.”
CORONAVIRUS LAYOFFS SURGE IN US, WITH 1 IN 5 HOUSEHOLDS REPORTING LOST WORK
Since the Affordable Care Act, aka ObamaCare, went into effect in 2010, 126 rural hospitals have shut down. Just last year, 19 rural hospitals closed their doors -- the highest spike since 2005, according to the North Carolina Rural Health Research Program.
“This year we’re on track to break the record,” said Maggie Elehwany, government affairs and policy vice president at the National Rural Health Association.
CLICK HERE FOR THE LATEST ON CORONAVIRUS
Rural health care providers say they are prepared for a reasonable surge in patients, according to Elehwany, but they will need access to the United States Department of Health and Human Services' stash of medical and pharmaceutical supplies should there be a national catastrophic pandemic.
“We need to make sure there’s an equitable distribution and find out proportionally where the pockets of the pandemic are,” Elehwany said. “If they’re in rural communities, we need to be ready to get some supplies to them right away.”
Texas leads the country in rural hospital closures, with 24 closings since Chartis Group starting tracking them in 2005. Of 152 rural hospitals in the Lone Star State, 77 are considered vulnerable based on annual operating margins and revenue. Forty-eight percent of rural hospitals in the state have negative operating margins.
CLICK HERE TO READ MORE ON FOX BUSINESS
As of Wednesday, there are 7,048 COVID-19 cases in the United States with 116 fatalities.