COVID-19 pushes rural hospitals to their limits
Nation’s smallest hospitals depend on larger facilities to care for their most complex patients, but larger hospitals are growing crowded
At the small hospital in Andrews, Texas, in the heart of America's oil patch, doctors had a critical patient this month who needed an urgent non-Covid-19 procedure that the smaller facility couldn't perform. Hospitals nearby had the right equipment and specialists but were overrun.
Physician Alyssa Tochterman of the 34-bed Permian Regional Medical Center made a pleading call to the chief executive of the closest large hospital. "Can you find someone to do this procedure?" she asked.
Dr. Tochterman then made an offer she wouldn't have considered before the pandemic: "We'll take him back," she said. The patient wouldn't stay after the procedure, as is normally the case, and would return to Permian Regional to recuperate.
"That's not how things are done," said Dr. Tochterman. She is one of four doctors at the rural hospital, which has no intensive-care unit. "Never in the history of ever" have small hospitals transferred patients to bigger facilities for procedures and immediately brought them back, she said. She was desperate, Dr. Tochterman said. It worked -- the patient got the procedure.
The trade-off is one of many that doctors and nurses at the nation's smallest hospitals are now making to help patients, as the pandemic's largest, most widespread U.S. surge pushes rural health care to its limits. Hospitalizations nationally have nearly doubled in November, setting a record Nov. 10, and every day since, to reach about 90,480 people in hospitals with Covid-19 on Thursday, Covid Tracking Project data show. The number of people in intensive-care units due to Covid-19 rose on Thursday to an all-time high of 17,802.

The number of people in intensive-care units due to Covid-19 rose on Thursday to an all-time high of 17,802. (iStock)
Early in the pandemic, hospitals and doctors had no available treatments, but have gained new therapies and more understanding of Covid-19 since then, which they say has helped to shorten hospital stays and improve survival. Still, the latest surge threatens to undo those advances as hospitals become overtaxed, doctors and health-care disaster-preparedness experts warn.
The prolonged surge has taken root in rural communities, straining small hospitals that are often vital waystations for patients who need to be transferred to larger hospitals with more specialists and equipment. Now, many larger hospitals are full.
Hospitals are busier now than during the nation's first surge in the spring, when they postponed large numbers of surgeries to free up nurses and preserve critical equipment for coronavirus cases. Sharp financial losses and backlogs of anxious patients followed, and many medical facilities are now attempting to continue more routine care even as Covid-19 cases climb.
NAIL SALONS FEAR FOR SURVIVAL DURING COVID-19’S LATEST SPIKE
Big hospitals are in some cases making room by sending patients to rural hospitals, where staff are keeping patients they normally wouldn't, either because they can't find an open bed elsewhere or because they are seeking to ease pressure on larger hospitals, said doctors, nurses and executives of hospitals in the Midwest and South.
The 10-bed hospital in Red Lodge, Mont., in October couldn't transfer an elderly patient with dangerously low oxygen levels who needed intensive care, said Kelley Evans, the hospital's CEO. "We met with the family and said, 'We're going to do everything in our power,'" for the patient, she said.
Doctors used their BiPAP -- or bi-level positive airway pressure -- breathing machine, which is less powerful than a ventilator, in an attempt to boost his oxygen levels, said Billy Oley, medical director of the hospital, Beartooth Billings Clinic. "It's all we have here. Without it, he would have died," Dr. Oley said. Physicians lacked the technology of larger hospitals and relied on laboratory work and close monitoring by doctors and nurses to make adjustments.
"It was definitely touch and go," Dr. Oley said. The patient survived and returned home.
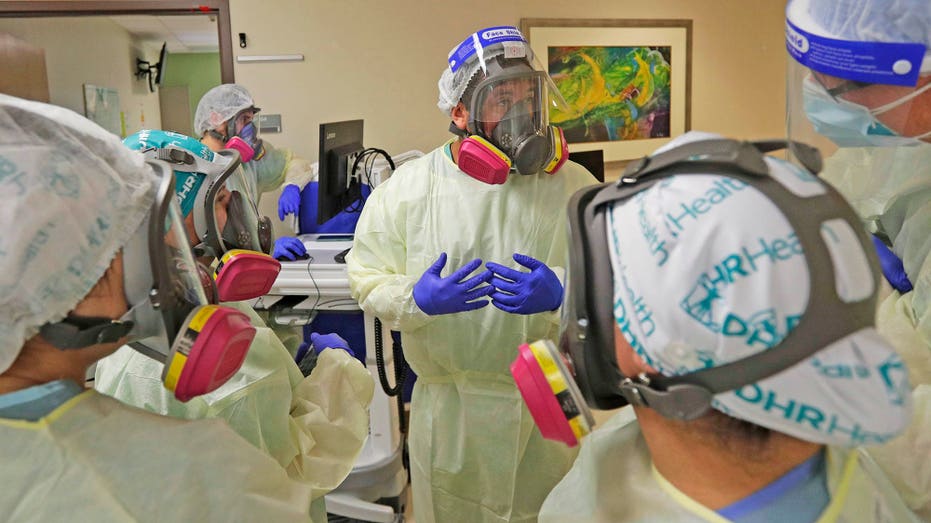
Medical personnel confer about COVID-19 patients in this file photo. (AP Photo/Eric Gay)
Large hospitals in North Dakota, Montana and Texas report that they must regularly deny smaller hospitals' transfer requests. Altru Health System in Grand Forks, N.D., has seen the number of transfers it must deny increase fivefold this year compared with the prior year, said a spokeswoman.
"Our ability to accept transfers changes hour by hour," said Katie Gallagher, a spokeswoman for St. Peter's Health Regional Medical Center in Helena, Mont.
In Texas, where the seven-day average of new cases has surpassed the summer surge and hospitalizations and deaths are rising, rural hospitals now make up to two dozen calls and send patients out of state to find an opening, say hospital officials there.
Hendrick Health's two large hospitals in Abilene, Texas, denied 100 transfers this month, including 30 in the past week, Kirk Canada, an assistant vice president with the system, said.
"There is nowhere to put them," said Russell Tippin, president and CEO of the Medical Center Hospital in Odessa, Texas, about 40 miles from Permian Regional. Mr. Tippin received Dr. Tochterman's mid-November call and agreed to the procedure because the rural hospital said its patient could quickly return. "That was huge," he said.
ASTRAZENECA MULLS ADDITIONAL TRIAL TO FURTHER INVESTIGATE COVID VACINE EFFICACY: REPORT
Midland Memorial Hospital in Midland, Texas, has been closed to transfers for much of the month, said its CEO Russell Meyers. "We're not far from reaching the end of our available resources," he said.
Patients swiftly filled the 36 new beds the hospital added two weeks ago. The facility gained 14 more beds for less-critical patients this week in a new medical tent.
Inside the emergency room, patients wait on stretchers and in chairs, and more patients must now remain there until beds become available, said Dana Taylor, Midland Memorial's director of emergency services.
Administrators could add capacity for another dozen patients on the hospital's ninth floor, but the hospital is waiting on equipment, including ventilator tubing and patient monitors, said the hospital's chief nursing officer, Kit Bredimus. Beds won't arrive until January. The hospital rented beds, which are scheduled to arrive next week.
More hospital capacity requires more skilled health-care workers to assist patients, in part because many hospital employees can't work after exposure to the virus.
Finding workers is increasingly difficult. More than 1,000 hospitals across the U.S. reported critical staffing shortages in recent days, U.S. Department of Health and Human Services data show.

Healthcare workers help each other with their personal protective equipment at a drive-thru coronavirus testing site. (AP Photo/Wilfredo Lee, File)
Some states have said hospitals and nursing homes can consider what the Centers for Disease Control and Prevention calls "crisis" or "contingency" staffing options, such as allowing workers to stay on the job after exposure or infection, under specific conditions.
University of Iowa Health Care in the past month relaxed restrictions to allow exposed workers without symptoms to remain on the job; workers are tested. Those who test positive stop working.
The system's University of Iowa Hospitals and Clinics in Iowa City, Iowa, include a 655-bed acute-care facility and 190-bed children's hospital. "If we didn't lift work restrictions, we would be denying patients care, " said CEO Suresh Gunasekaran.
Altru Health is considering ways to safely bring asymptomatic workers with Covid-19 back on the job to work with coronavirus patients after the state's governor amended an order to allow it, said Janice Hamscher, Altru's chief nursing officer.
GET FOX BUSINESS ON THE GO BY CLICKING HERE
"In order to safely care for all patients who need us, we must consider this option to do so," Ms. Hamscher said. "Our staff are not immune to community spread." Altru hasn't yet asked Covid-19-positive employees to return to work under the new order.
With the rise in local cases in recent weeks, the Winkler County Hospital District in Texas is unable to transfer patients to Odessa, which is where Winkler County Hospital typically sends most patients. It now takes longer to find a bed, and patients travel farther to hospitals in New Mexico's Santa Fe and Albuquerque, or within Texas to Amarillo, Fort Worth, Abilene, San Antonio and El Paso, before El Paso saw its own surge.
In the Kermit, Texas, hospital, emergency-room nurse Sharla Mitchell has made more than two dozen calls to find a bed for a critically ill patient, turning to Google to find out-of-state hospitals able to accept transfers, she said.
"It's really scary," she said. "I don't know what's going to happen the day we can't find a bed."




















