Hospitals prepare to lose staff over COVID-19 vaccine mandate
Some workers are required to be vaccinated by Jan. 4
Fox Business Flash top headlines for November 29
Check out what's clicking on FoxBusiness.com.
Some hospitals, nursing homes and other healthcare providers are preparing to operate without up to a third of their staff at the start of next year, if those workers don’t comply with a federal mandate to get vaccinated against COVID-19.
The Biden administration is requiring facilities that receive funding from the Centers for Medicare and Medicaid Services to have workers vaccinated by Jan. 4. Two dozen states are challenging the requirement in court. Many healthcare providers in those states and beyond are reviewing requests for religious and medical exemptions from the rule or firing workers who won’t get the shots.
Some health care employers are setting a hard line against exemptions, betting that will encourage more workers to get vaccinated. Others are being more permissive. And some are looking to hire workers who have left or been denied exemptions at other hospitals and clinics. The decisions add up to a major operational threat for some healthcare providers at a time when workers are in shorter supply than ever.
VARNEY: OMICRON IS A TEST OF THE BIDEN PRESIDENCY

President Biden spoke from the White House Monday Nov. 29, 2021, just days after the World Health Organization designated omicron a "variant of concern," its most serious designation of a COVID-19 variant.
Thirty percent of workers at more than 2,000 hospitals across the country who were surveyed in September by the Centers for Disease Control and Prevention were unvaccinated. Applied to a nationwide healthcare workforce of some 22 million according to the Census Bureau, that would equal nearly seven million who have yet to get inoculated.
Some 17 million healthcare workers are employed at facilities that receive reimbursement from the federal Medicare and Medicaid programs, according to CMS. The Biden administration earlier this month made future reimbursement contingent on all eligible staff getting fully vaccinated against Covid-19 by Jan. 4. The regulation allows for medical and religious exemptions.
Hospitals and recruiters say a combination of exemptions and more workers choosing to get vaccinated in the coming weeks should help alleviate the operational threat. Some facilities said they didn’t expect operational disruptions. But in some rural areas, the loss of one or two employees can crimp a facility’s ability to provide care, doctors and hospital operators said.
Clark Fork Valley Hospital and Family Medicine Network in Plains, Mont., won’t be able to provide basic medical care in an area 90 miles from any larger hospital centers if more employees don’t get vaccinated, said Nick Lawyer, who practices family medicine there.
"It would mean a tremendous reduction in service," he said.
About 55% of the hospital’s 200 employees are vaccinated, Dr. Lawyer said, even after hospital leaders held sessions encouraging more of them to get the shots. The full vaccination rate in surrounding Sanders County is about 36%.
The hospital gets approximately 85% of its funding from CMS, Dr. Lawyer said. He said the hospital was considering giving workers wide leeway to apply for religious exemptions. He said he wasn’t sure it would be enough to retain the workers necessary to avoid service cuts.
Groups that advocate for religious freedom including Liberty Counsel, Thomas More Society and the Center for American Liberty said they have received thousands of requests for assistance from people who have been denied religious exemptions to Covid-19 vaccine mandates. The groups have filed lawsuits on behalf of healthcare workers fighting vaccine mandates.
Condon McGlothlon, a partner and employment-law specialist at Seyfarth Shaw LLP, said no one anticipated a situation where thousands of employees across the country would simultaneously request religious exemptions. He said employers are weighing the staffing crunch if they lose unvaccinated workers against the risk to the health of other employees if those people stay.
In places where mandates have already gone into effect, vaccination rates have risen by 20 percentage points, a recent White House report found. Before the CMS mandate, more than 2,500 hospitals, 40% of the nationwide total, had set vaccination requirements for workers, according to the report.
"We did this months ago," said Houston Methodist Chief Executive Officer Marc L. Boom.

U.S. President Biden removes his face mask as he arrives to speak in the South Court Auditorium on the White House campus Oct. 14, 2021 in Washington, D.C. (Drew Angerer/Getty Images / Getty Images)
Roughly 85% of the more than 26,000 staffers at Houston Methodist were vaccinated by the time the hospital’s mandate took effect in March, leaving leaders to try to persuade the remaining 15% and to evaluate requests for medical and religious exemptions. Many who had taken flu shots in previous years applied for religious exemptions from the Covid-19 vaccine, requests that were largely denied.
CLICK HERE TO READ MORE ON FOX BUSINESS
Less than 1% of staff left rather than comply, Dr. Boom said, including nurses, respiratory therapists, accountants and IT staffers. He said the nearly 100% vaccination rate among remaining staff helped insulate Houston Methodist from the worst of the summer surge driven by the Delta variant.
Still, places with acute staffing shortages are showing signs of operational strain. In New York, which set a Sept. 27 deadline for healthcare staff to get their first vaccine doses, upstate Lewis County Health System recently paused maternity services because of the number of employees refusing to get vaccinated. The state isn’t allowing religious exemptions, a stance that has been challenged in court. A federal judge ruled last month that the state must allow people to seek religious accommodation while the suits proceed.
In Maine, which isn’t allowing religious exemptions, the Maine Health Care Association said five nursing homes and one assisted-living facility have closed since the statewide mandate for healthcare workers was announced in August. The group estimates that up to 10% of nursing-home workers will leave rather than comply with the mandate. Healthcare workers who have refused the vaccine on religious grounds have organized a legal challenge. The state was already experiencing an acute healthcare-worker shortage before the pandemic. Despite vaccination compliance above 95% in most hospitals, operating with even a partially diminished staff has reduced service in parts of the state.
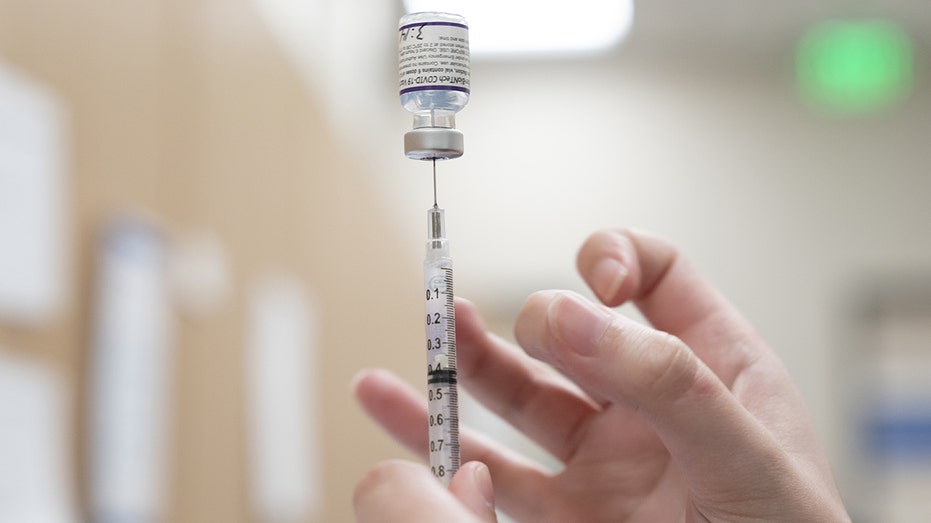
A health care worker prepares a dose of the Pfizer-BioNTech Covid-19 vaccine at an Oklahoma County Health Department Vaccine Clinic in Oklahoma City, Oklahoma on Nov. 17, 2021. (Nick Oxford/Bloomberg via Getty Images / Getty Images)
CLICK HERE TO GET FOX BUSINESS ON THE GO
Garth Berenyi, from Levant, Maine, who was fired last month from the nursing home where he worked as executive director because he declined to get vaccinated, said he would likely look for work in another state. He said he objected to aborted fetal cell lines used in the testing or development of vaccines. All three Covid-19 vaccines cleared for use in the U.S. made use during testing or production of cell lines grown in laboratories based on aborted fetal cells collected decades ago.
"My conviction is clear. I’d be sinning if I did that. It goes against every fiber in my being," said Mr. Berenyi.




















