Combating Preventable Rehospitalizations: No Easy Task
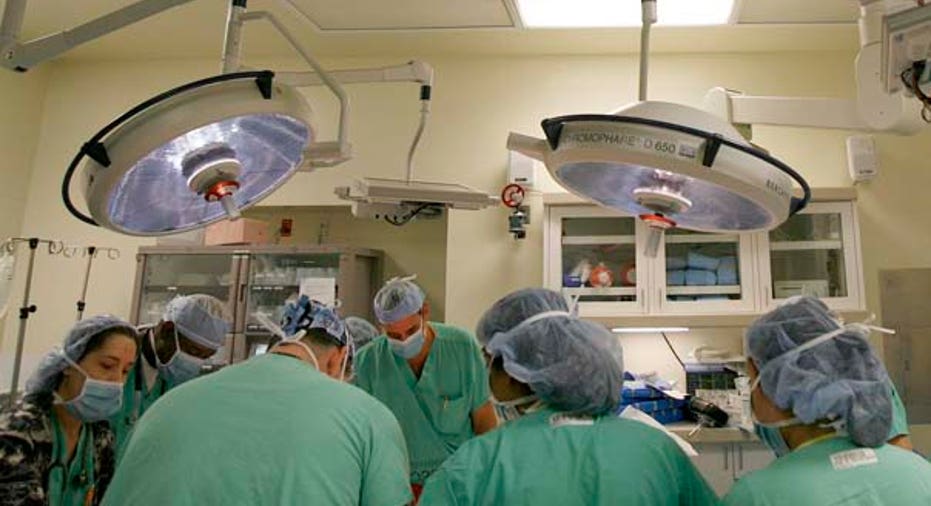
The frequency of patients returning to hospitals soon after being discharged is a problem plaguing the American health-care system at an estimated cost of $12 billion in Medicare spending and $25 billion across all payers annually.
According to the Institute for Healthcare Improvement (IHI), approximately five million rehospitalizations occur each year, and non-Medicare numbers are roughly equal.
Whats even more staggering is experts estimate that 76% of the readmissions are preventable.
Patients are in the worst kind of maze, one with hazards, barriers and burdens, says Rebecca Bryson, a patient from Whatcom County, Wash. She suffers from diabetes, cardiomyopathy, congestive heart failure and several other complications and at one time saw 14 doctors and took 42 medications.
Parts of the Patient Protection and Affordable Care Act (PPACA) may help patients like Bryson navigate the system successfully and prevent repeat hospital visits. The new health-care law includes opportunities and incentives such as instituting a community-based care transition program between 2011 and 2015, and the identification, evaluation and dissemination of innovative care delivery and payment models between 2011 and 2019. But these programs dont come cheap with some estimating a cost of $500 million and $10 billion.
Tackling the problem state by state
There is also growing momentum of state and organizational initiatives to create novel solutions to rehospitalizations without mandates. One such endeavor is a four-state initiative launched in 2009 by IHI and supported by a grant from the Commonwealth Fund.
The State Action on Avoidable Rehospitalizations initiative, STAAR works to improve care transitions (e.g., the movement of patients out of the hospital, into a skilled nursing home, sub acute facility, or the home) to reduce rates of avoidable rehospitalizations in Massachusetts, Michigan, Ohio and Washington.
STAAR looks at infrastructure around care transitions from a state leadership perspective. Two years into its four-year cycle, 148 hospitals are working in partnership with more than 500 cross-continuum team partners.
With a strong reliance on technology, stakeholders are working to accomplish STAARs mission without adding extra cost for human resources, says Patricia Rutherford, IHI vice president and co-principal investigator for the STAAR initiative. It is not sustainable to add extra cost.
It may be too soon to reference publicly-available data that shows whether STAAR is achieving its primary goal of reducing avoidable hospitalizations, but so far the effort has shown to be successful.
Up to this point, the majority of successful approaches to reducing rehospitalizations occurred under conditions in which hospitals received financial incentives, engaged in financial gain-sharing arrangements with payers, or focused inward to make explicit organizational investments in new service models, including hiring new staff to provide education, coordination and outreach. It takes a village to do this work, says Rutherford.
STARR acts on multiple levels with the hospital, the community, the state, as well as nursing facilities, community-based care providers, home-health agencies and patient and family representatives to improve communication and coordination during patients transition between care settings.
Surprisingly, 20% to 25% of hospital readmissions occur at hospitals different than the ones from which patients have been discharged, according to Rutherford.
To better track repeat patients, STARR teams must perform chart reviews and interview five recently- readmitted patients to identify missed opportunities and ways to improve transitions. Who better to ask what happened and what went wrong but patient families and patient care providers and the patients?
The hallmark of patient-centered care is the journey, says Rutherford. What is the patients life like in the year following a hospitalization?
While competent and hardworking, individual providers are too frequently operating in silos, Rutherford says.
Bryson can attest to that. In addition to having to understand her multiple conditions and treatments, she was the sole communicator among her numerous providers, passing information to each one after every admission, appointment and medication change.
A patients ability to restate his or her care requirements is a key indicator of success post-hospital. One way to do this is to improve the hospital discharge process, a practice that actually is reliant on robust information gathering with teach back at a patients hospital admission.
A handover of patient information at discharge helps combat the all-too-often occurrence of transfer paperwork arriving two weeks following discharge. This model is already showing success in Washington State where a standardized patient communication tool, a web or paper-based document, has been implemented through a partnership between some state hospitals, its hospital association, medical and pharmaceutical associations and community health care providers.
In Washington, the enhanced role of the clinical care specialist makes a nurse or social worker a patients coach, advocate and guide.
Also, the Massachusetts Care Transitions Forum has aligned many complementary care transition activities across the state along with STARR.
Different care settings have specific tools to improve processes within their own settings, even as they work to improve communication across organizations, says Rutherford. The key is to create, package and hardwire ideas into daily practice.



















