Surprise! Here's What Would Happen if Congress Raised the Medicare Eligibility Age
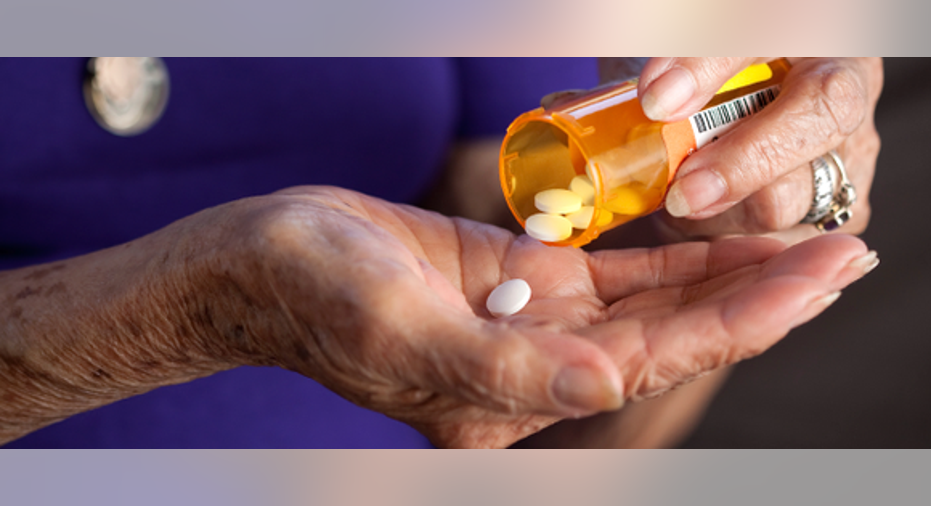
Medicare may grow to become the most important entitlement program for seniors in the coming decades. As medical costs increase, the cumulative lifetime benefits received from Medicare could one day surpass the lifetime benefits seniors receive from Social Security. Thus, the future of Medicare is critical for the 40 million seniors currently covered by the program, as well as the countless millions who'll become eligible in the coming years.
Medicare is in trouble But Medicare has some serious issues to contend with. While designed to help seniors aged 65 and up cover approximately 80% of their eligible medical costs, the program simply isn't bringing in enough revenue via the payroll tax to cover its long-term costs. Based on the latest report from the Board of Trustees, the Hospital Insurance Trust is projected to exhaust its cash reserves by 2030 (or sooner if medical cost inflation is higher than expected). If this were to happen without any reforms being made by Congress, reimbursements to hospitals and physicians would be reduced to the amount of revenue being brought in on a monthly basis.
Change is needed to ensure the program survives for many years to come and is capable of sustaining today's benefit levels. Thus far, an amicable solution to fix Medicare has eluded lawmakers.
One of the most commonly proposed fixes for Medicare is raising the eligibility age for the program from 65 to 67. The logic behind the move is pretty easy to understand. Since we're living longer than ever before, according to the Centers for Disease Control and Prevention, it would presumably save Medicare (and the federal government) money if Americans were required to maintain private insurance for an additional two years before becoming eligible for Medicare. In fact, estimates from the Congressional Budget Office have suggested that raising the eligibility age to 67 from 65 would save $17.1 billion per year in 2023. If subsidies and other revenue losses were taken into consideration, the net benefit is pegged at cost savings of $6.7 billion.
Image source: Pictures of Money via Flickr.
But just how practical of a solution is this? Based on the findings of a new study published in Health Affairs this week, raising the Medicare eligibility age could have a surprisingly undesirable result.
Raising the Medicare eligibility age: not so smart after all? The authors of the study were Jacob Wallace, a doctoral candidate in health policy at Harvard, and Zirui Song, a resident physician at Massachusetts General Hospital and clinical fellow at Harvard Medical School. The two researchers examined how consumer spending differed between Medicare and private insurance when switching to Medicare at age 65 using Truven Health Analytics data on outpatient imaging and medical procedures. What the researchers found was that healthcare spending dropped by $38.56 per beneficiary per quarter, or 32.4%, when signing up for Medicare at age 65. Of note, this study did not factor in the effects of Medicare Advantage plans.
In simpler-to-understand terms, researchers determined that consumers save a substantial amount of money moving from private insurance to Medicare at age 65. Conversely, they observed that pushing the eligibility age out to 67 would actually increase costs since the consumer would be more reliant on higher-cost private insurers that probably don't offer the broad array of services that Medicare does. Researchers suggest that $3.7 billion in out-of-pocket expenses could be shifted to consumers, with another $4.5 billion in cost increases falling on employers who cover the medical expenses of retirees.
Perhaps the most interesting finding from the study was that the 32% decrease in spending when switching from private insurance to Medicare had little to do with a lower medical utilization rate or from providers turning down Medicare coverage. Instead, the authors contend that Medicare's sheer size allows it to contract with providers at a reduced rate. In other words, Medicare's size gives it purchasing power advantages that substantially help it control costs for consumers relative to private insurance.
Long story short, raising the eligibility age could prove devastating to seniors, and may cost more than it saves.
Image source: Flickr user Francisco Osorio.
Medicare's best solution could be its toughest to implement So, what's the best way to fix Medicare? Although there is no bona fide quick fix, the best solution involves shifting away from traditional fee-for-service care, whereby physicians get reimbursed for providing a service to a patient, to a value-based system that rewards physicians who provide meaningful care to a patient. Under the sustained growth rate model, physicians are encouraged to provide testing and services that might otherwise be unnecessary since they're reimbursed for each service rendered. Under a value-based system, payment is based on patient outcome, with better patient outcomes yielding higher reimbursements for physicians.
For example, every hospital readmission that's avoided saves the healthcare system between $10,000 and $13,000, and the patient also experiences better quality of life, per Forbes.
The biggest challenge, though, is defining what's meant by the term "value" and how to reward it. Physicians need to be properly incentivized to provide the right care and rewarded when they achieve a positive outcome. Conversely, they should be penalized when achieving a poor result. However, physicians also need to be given the appropriate tools to help improve their chances of success. This means from top to bottom there have to be stakeholders with a vested interest in improving the quality of patients' lives. Defining "value" and finding the right payment model simply isn't going to be easy.
Image source: U.S. Food and Drug Administration.
The most recent example of the value-based model in action can be seen in a series of experimental changes to Medicare Part B drug reimbursement in select markets. Traditionally, Part B pays the average selling price of a drug plus a 6% add-on rate. Presumably, this would entice physicians to prescribe the most expensive drug, since it would result in the biggest add-on payment. However, the most expensive drug may not be the best drug for the patient (or their wallet).
The solution was to reduce the add-on rate to 2.5% and add a $16.80 flat-fee payment per drug on top of it. This move increases the reimbursement rates on drugs in the $5 and $10 range by 339% and 171%, respectively, encouraging physicians to consider the full gamut of therapies available when treating their patients.
It remains to be seen whether this transition to a value-based model can be made with ease, or if change will continue to be met with resistance by physicians and select advocacy groups. The only thing for certain at the moment is that Medicare's current path is unsustainable, and we have perhaps 14 years, or less, to fix it.
The article Surprise! Here's What Would Happen if Congress Raised the Medicare Eligibility Age originally appeared on Fool.com.
Sean Williamshas no material interest in any companies mentioned in this article. You can follow him on CAPS under the screen nameTMFUltraLong, track every pick he makes under the screen name TrackUltraLong, and check him out on Twitter, where he goes by the handle@TMFUltraLong.The Motley Fool has no position in any of the stocks mentioned. Try any of our Foolish newsletter servicesfree for 30 days. We Fools may not all hold the same opinions, but we all believe thatconsidering a diverse range of insightsmakes us better investors. The Motley Fool has adisclosure policy.
Copyright 1995 - 2016 The Motley Fool, LLC. All rights reserved. The Motley Fool has a disclosure policy.



















