It's Time to Change the Organ Donor Policy
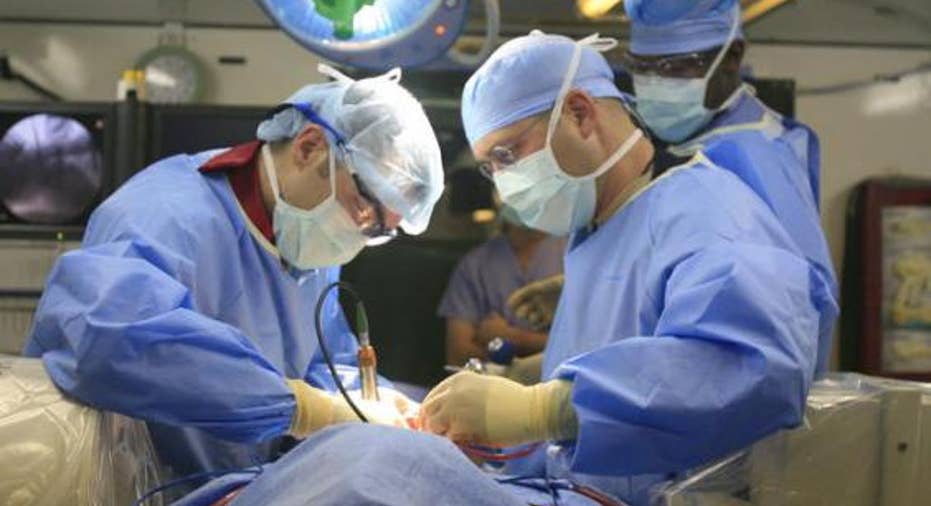
Watching Sarah Murnaghan, the 10-year-old with end-stage cystic fibrosis, and her mother beg for consideration to receive a lung from the adult donor list has been heart-wrenching. It’s been unlikely that Sarah would receive a lung from the under-12 list because there are so few donors in that age category. Sarah’s mom has urged officials to make an exception as her young daughter’s condition continues to deteriorate. Last night, a U.S. district court judge agreed, and put her on the list, although a hearing later this month could call into question that decision.
Is that the end of the story? Far from it. Bioethicists and others are raising questions about the fairness of the judges’ ruling. What about the people who were already on the list to receive a new lung? Even though we haven’t seen their faces in television packages and on newspaper covers, their plight is no less pressing.
The workings of donor lists is a mystery to most of us. What is clear is this: there are simply not enough organs to go around. One simple change would be to make organ donation the law of the land, unless an individual decides to opt out for whatever reason, religious or otherwise. You would be “opted in” automatically to donation, unless you chose to “opt out.” Let’s face it, many of us believe in donation, but simply don’t get around to checking the box on our drivers’ license that would allow our bodies to be used to help other people. If the law were changed to make organ donation automatic, the shortfall of organs would be solved and lives would be saved.
A friend of mine watched in horror as her brother’s bid for a new heart failed. She says the system doesn’t work and needs reform.
Mercedes Colwin, an attorney and Fox News contributor, told me, “Unfortunately, my 41 year old brother Arthur was a victim of the organ donation process. Balancing all the competing concerns – the medical care being administered, the grim diagnosis, the family life in tatters – is overwhelming for anyone facing a transplant. Simplifying the process and eliminating delays while maintaining the best medical care for these patients must be a priority. This can be accomplished through an opting out process as opposed to opting in for organs. Currently, overwhelmed families and patients must confer with their doctor and make the already difficult time sensitive choice of being placed on a transplant list. Ultimately, the process becomes a race for organs as the timing of when the patient is placed on the list becomes a significant factor, sometimes eclipsing medical necessity. In an opting out process, the patients will be placed automatically on a transplant list and the patient has the choice to remove themselves from the list. In my own family, Arthur battled heart disease for two years before he was placed on a list. With only weeks to live, there was no heart to save him. “
We know there is a better policy for organ donation. We should make the simple change that could save thousands of lives.



















