Innovation in Surgery: Getting People Back to Work Faster
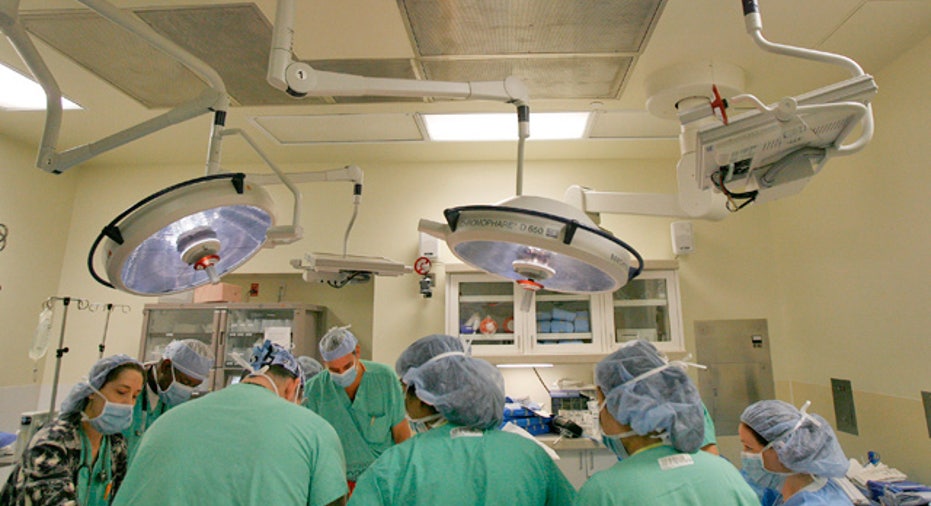
The weak economy and anemic labor market have caused many Americans to put off necessary treatments and surgeries due to fear of missing work or not being able to afford the medical bills. But new technologies could change the health-care landscape and enable people to undergo less invasive surgical procedures and experience a faster recovery and return to work quicker.
For example, some older patients are so put off by high deductibles that they are putting off knee replacement surgery and enduring knee pain until age 65 when they’re on Medicare. But young patients are also delaying treatments over fear of costs and lack of health insurance.
According to Dr. John Tongue, an orthopedic surgeon and president elect of the American Academy of Orthopaedic Surgeons, economic considerations have undercut many patients’ objectives to eliminate pain, regain mobility and stay active to improve overall long-term health.
The high unemployment rate means many Americans are without health insurance and tend not to be able to afford costly surgeries. Employed workers are also putting off medical treatments due to fear of the potential financial burden created by time out of work, not to mention a fear that the time off for recovery will cause them to lose their jobs, Tongue says.
With this fear in mind, many companies are working to create new technology that will reduce a patient’s recovery time.
Musculoskeletal care company Zimmer has personalized joint replacement technology that enables improved surgeon dexterity when performing procedures and helps patients bounce back more quickly..
One relatively young company, ConforMIS, along with patient specific instrumentation, has introduced iTotal, a customized patient knee that conforms to a patient’s specific anatomy. The customization is made possible based on CATS or MRIs taken before the surgery.
“What I’m used to seeing in three months, I now see in a six-week follow up”
According to Dr. Philipp Lang, ConforMIS founder and president, “Current implants are limited in fit.” The implant used on a petite, small-framed woman can’t be used on a taller, large-boned male.
Customization makes the procedure less invasive, as less bone and ligaments are cut to achieve an appropriate fit.
JFK Medical Center’s Dr. Gregory Martin says iTotal’s “less is more approach,” translates to a shorter recovery time. “My patients are back to work more quickly; there’s less pain medication required and their rehabilitation time is cut in half.
“What I’m used to seeing in three months, I now see in a six-week follow up,” Martin says.
Lang says the iTotal procedure is also cost competitive for patients because it reduces the length of their hospital stay.
Beyond knees
Alex Morozov, a health care analyst at Morningstar, says technological medical advancements over the past decade in other areas of surgery are also moving toward more minimally-invasive procedures that drastically reduced recovery time. “Lots of companies are striving to minimize collateral damage to a patient’s body and to decrease the number of days patients need to recuperate. They are moving further away from an open surgical environment to a less invasive process.”
In gynecology, for example, companies like Conceptus and Adiana have introduced minimally- invasive procedures for female permanent sterilization procedures that are done in office and result in limited, if any, down time from work.
Using robotics in surgery has also taken off, according to Morosov. Intuitive Surgical’s innovations in this area have reduced the invasiveness of procedures like a hysterectomy, and the company is looking to improve surgical outcomes through robotics in the neurovascular area.
Nonelective areas made simpler and faster
Endovascular surgery is already changing the surgery landscape when it comes to aneurysms, according to Dr. Cameron McDougall, president of the Society of NeuroInterventional Surgery.
Endovascular surgery is much less invasive and involves a soft coil being inserted into the femoral artery and maneuvered delicately to the brain where the aneurysm is packed with platinum coils until it is sealed off. The traditional platinum coil with its PGLA polymer on its outside t is designed to degrade over time and promote rapid tissue development within the aneurysm.
This procedure is being used in appropriate cases instead of a craniotomy in which the top portion of the skull is removed and the aneurysm is clipped and the skull replaced, according to Mark Paul, president of Stryker Neurovascular that developed the technology.
The reduced healing time with the coil compared to the craniotomy is quite significant—two or three days in the hospital as opposed to five or 10 with the open surgery, says Paul.



















