How smart technologies can revamp Medicaid systems
This content is from our sponsor. Fox Business editorial was not involved in the creation of this content.

Making even minor upgrades to a system as large and as complicated as a legacy state Medicaid program would be expensive and time-consuming, potentially even requiring an entire system overhaul. Considering the size and scope of a Medicaid system, adopting smart technologies would go a long way towards modernizing these programs.
A Medicaid system that harnesses smart technologies has the potential to transform the way Medicaid agencies work. Imagine a Medicaid system—enabled by smart tools—that can sift through massive amounts of patient data, recognize patterns, and help predict a member’s future health outcome; or improve access to managed care because the network is assessed with geospatial information systems (GIS).
In “Smart Medicaid,” Deloitte explains four key areas in which smart technologies can help Medicaid programs, addresses barriers to adoption, and provides tips for implementing a smart Medicaid system.
A Smart Medicaid System
Legacy Medicaid systems have been using Medicaid management information systems (MMIS), which are massive, hard-coded platforms that are impractical to upgrade. Going forward, though, the Centers for Medicare and Medicaid Services (CMS) are creating more technologically flexible and agile systems by implementing interoperable modules with a common security infrastructure.
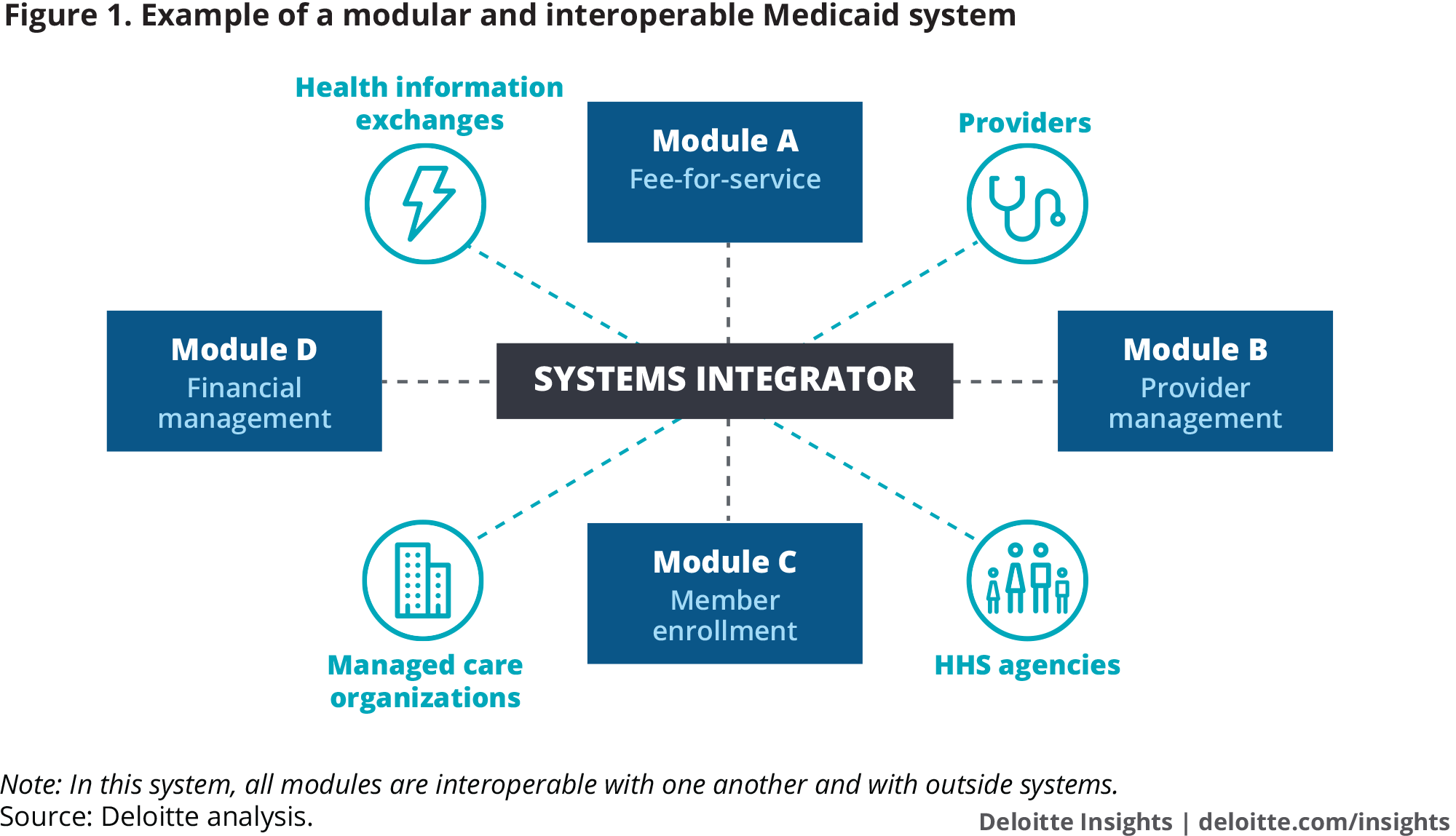
Deloitte illustrates this setup perfectly, explaining: “It might be helpful to think of a modern Medicaid platform as a smartphone, and the modules as smartphone apps. Just like apps, modules can be added, deleted, or updated as needed without upgrading the entire smartphone.”
Interoperability means these modules can communicate with each other, sharing data and functionality, and all modules in these modern systems will be interoperable with each other and with outside systems.
Deloitte specifically references two significant architectural evolutions that a Medicaid system should take advantage of in order to become a smart platform:
Open APIs - An API (application programming interface) allows pieces of software to interact with each other, and when “open,” authorized users can be granted access. Logging into a site like Airbnb using your Google credentials—which is time-saving and secure—is possible because of an open API by Google.
Older Medicaid systems cannot use this method for sharing data with external systems, but with Smart Medicaid systems that enable APIs, this can be done easily.
Cloud computing - Some states are migrating their Medicaid platforms to the cloud [i], allowing them to take advantage of the cloud’s storage capabilities while also easily and affordably incorporating cloud-based applications like artificial intelligence and machine learning tools.
Smart Technology Examples
Smart technology can help a Medicaid program run more efficiently—saving money while better serving their state’s population—but they need to be integrated into a cohesive framework to solve the major problems.
Internet of Things (IoT) technology, machine learning, and geographic information systems (GIS) are three types of smart technologies that Deloitte believes can help Medicaid programs in a few key areas:
- Promotion of independent living - IoT technology has made remote patient monitoring (RPM) possible, meaning that elderly patients who want to continue living independently can have vital statistics—like glucose levels, exercise, and whether they’ve taken their medication—monitored in their homes.
- Program operations - IoT technology can be used to alleviate the inefficiencies of non-emergency medical transportation (NEMT) services by monitoring pick-ups, wait times, and drop-off locations—reducing late and missed appointments and lowering program costs by monitoring for fraud and waste.
- Customer service - Machine Learning and cloud computing provide the opportunity for agencies to integrate chatbots that can learn to respond to queries, complete forms, or present explanations in simpler terms for members who need help.
- Targeted interventions -- GIS can be used to map out “super utilizers,” to determine what factors could be associated with their poor health, while machine learning techniques could potentially predict members who are likely at risk of being hospitalized. Steps can be taken to prevent or alleviate their conditions or provide treatment and education.
Getting Started
Security and financing are two barriers to adoption that need to be addressed when considering a smart Medicaid program. The CMS is supporting efforts to upgrade and develop smart MMIS systems through federal matching funds[ii], so states should consider inquiring about specific costs that can be funded by federal contributions.
The safeguarding of medical information, which is required by the Health Insurance Portability and Accountability Act (HIPA), would be addressed in a modular and interoperable system by a common security infrastructure that provides for the safe exchange of data between modules and external systems. Installing firewalls, encrypting data streams, and regularly changing passwords are also important.
Agencies looking to get started creating a smart Medicaid system should consider the following tips:
Upgrade your platform - upgrade to a modular and interoperable platform with open APIs and leverage the cloud.
Start small - start slowly with one smart technology at a time and gradually work up to more complex projects that may require multiple technologies working together.
Develop a cohesive framework - build a comprehensive blueprint of the whole smart system—including how the technologies will perform and interact.
Use analytics to monitor outcomes and ROI - evaluate outcomes and return on investment with data and analytics to generate future returns on the upfront investment needed to upgrade to a smart system.
Establish a process for continually evaluating new technologies - constantly evaluate whether the latest smart technologies can further improve Medicaid operations.
Click Here for More Insights from Deloitte
Authors: Melissa Majerol, William Carroll, Sally Fingar
[i] Roger A. Maduro and David Perara, “Wyoming is taking Medicaid to the cloud,” Open Health News, January 1, 2017; Steven Ross Johnson, “Two for the price of one,” Modern Healthcare, October 19, 2013.
[ii] Vikki Wachino, letter to state Medicaid directors, accessed December 2, 2017.



















