Hospital Quality Measures May Miss the Sickest
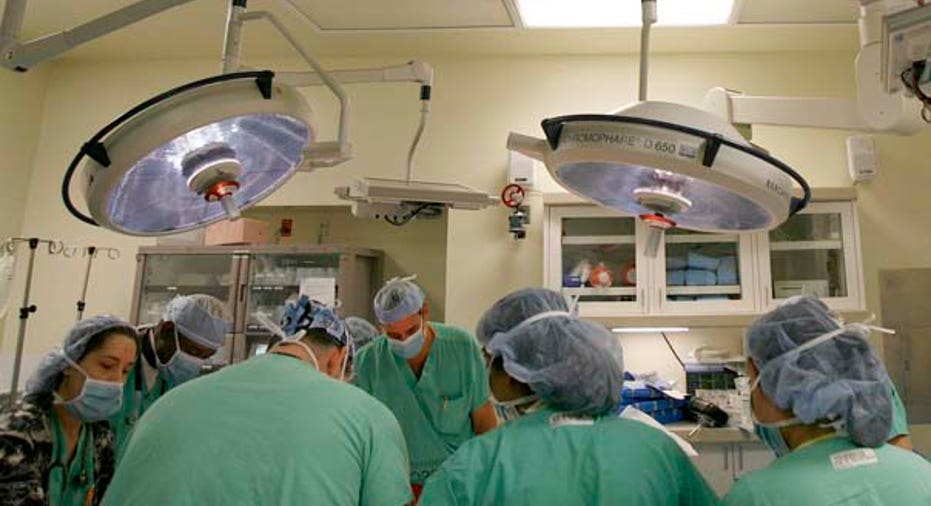
Public measures of hospital quality may not reflect care for the sickest patients -- or even the majority of patients in some instances -- suggests a new study of heart attack cases.
As a result, the researchers caution that quality-of-care rankings -- accessible through Medicare's Hospital Compare website-- likely don't tell the whole story about how well a hospital is doing.
The quality of care at U.S. hospitals is under great scrutiny, perhaps now more than ever because of growing interest by policymakers in linking treatment costs and benefits. Among the ways to gauge care is to determine how often a hospital provides standard treatments that have been shown to work well in research studies, such as giving aspirin or beta-blockers to patients undergoing treatment for a heart attack.
"But sometimes patients who come into the hospital with a heart attack have other medical conditions that mean that the standard treatments are not right for them," lead researcher Dr. Susannah M. Bernheim of Yale University, New Haven, Connecticut, told Reuters Health in an e-mail.
Current rules allow for these patients to be left out of reports that are required of U.S. hospitals to receive their Medicare payments. This exclusion is automatic under certain conflicting conditions, such as an allergy to the medication; in fuzzier cases, the decision falls under the discretion of doctors.
Bernheim and her colleagues identified three sets of hospital data on more than 200,000 Medicare patients admitted for acute myocardial infarction (heart attack) between 1994 and 2001, and then looked at trends in the use of five standard treatments: aspirin or beta-blockers at admission and at discharge, as well as ACE inhibitors at discharge for patients with a particular heart ventricle dysfunction.
While today's reporting rules were not yet in place at the time, the researchers found that the percentage of patients with conditions that could now lead to their exclusion from the quality reports under the "discretionary" rule increased across three periods covered by the data.
Of those who would not have been automatically excluded in 2000 and 2001, for instance, between a quarter and more than two thirds of heart attack patients had a condition complex enough to have led to their discretionary exclusion, report the researchers in the American Heart Journal.
Further, the researchers found that almost no patients were clearly appropriate for all five of the standard treatments.
"This means that such quality measures are not measuring care for all patients," said Bernheim, noting that the missing patients are often the sickest -- typically older and suffering from multiple medical conditions.
"There's a potential for hospitals to use the exclusions to make themselves look better on the quality measures, but you can't say that for sure based on what we've studied," she added.
Bernheim pointed out that the findings also highlight a gap in scientific knowledge and suggest a need for more research focused on determining the best treatments for ambiguous cases, as well as the development of better quality measures that reflect the care provided to all patients.
"I also believe publicly reported quality measures should include information about how many patients are excluded from the measure," she added.



















