Pfizer’s COVID-19 vaccine 95% effective in final results, company to seek approval within days
Pfizer to seek authorization within days, after companies report shot showed signs of being safe
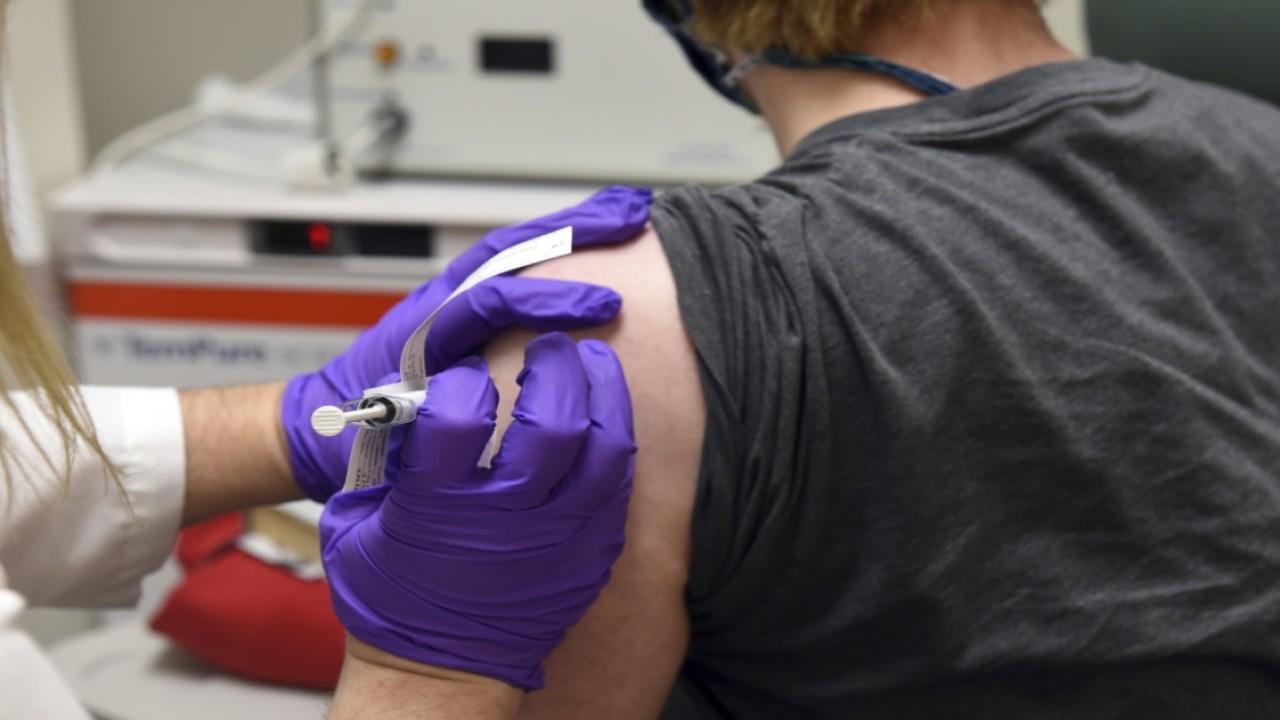
An experimental COVID-19 vaccine from Pfizer Inc. and BioNTech SE was 95% effective in final results from a pivotal study and is showing signs of being safe, key pieces of data as the companies prepare to ask health regulators to authorize use.
Pfizer plans to seek authorization for the vaccine within days, the companies said Wednesday, leaving the vaccine on track to go into distribution by the end of the year if approved by health regulators.
PFIZER TO START PILOT DELIVERY PROGRAM FOR ITS COVID-19 VACCINE IN FOUR STATES
| Ticker | Security | Last | Change | Change % |
|---|---|---|---|---|
| PFE | PFIZER INC. | 25.87 | +0.06 | +0.23% |
| BNTX | BIONTECH SE | 93.66 | +0.32 | +0.34% |
Out of 170 adult volunteers in the nearly 44,000-subject trial who developed Covid-19 with at least one symptom, 162 received a placebo, while eight got the vaccine, Pfizer and BioNTech said.
The resulting 95% effectiveness rate puts the shot's performance on par with shingles and measles vaccines. It is also consistent with the vaccine's showing in a peek last week at how it did in an analysis of the first 94 subjects to fall sick.
PFIZER-BIONTECH VACCINE CREATOR SAYS LIFE COULD RETURN TO ‘NORMAL’ NEXT WINTER
Researchers haven't found any serious safety issues, the companies said. The vaccine appeared to be well tolerated following a review of data from 8,000 study subjects, the companies said.
A severe side effect was fatigue, reported by 3.8% of the subjects, the companies said. Also, 2% of subjects reported headaches.
The companies said they have collected the two months of safety data on about 19,000 study subjects requested by the U.S. Food and Drug Administration but are still reviewing all those results.
PFIZER-BIONTECH CORONAVIRUS VACCINE EXPECTED TO PROTECT PATIENTS FOR A YEAR: CEO
"The study results mark an important step in this historic eight-month journey to bring forward a vaccine capable of helping to end this devastating pandemic," Pfizer Chief Executive Albert Bourla said. "We continue to move at the speed of science to compile all the data collected thus far and share with regulators around the world."
The company is waiting to fully analyze the data and compile required documentation before asking for authorization, a spokeswoman said.
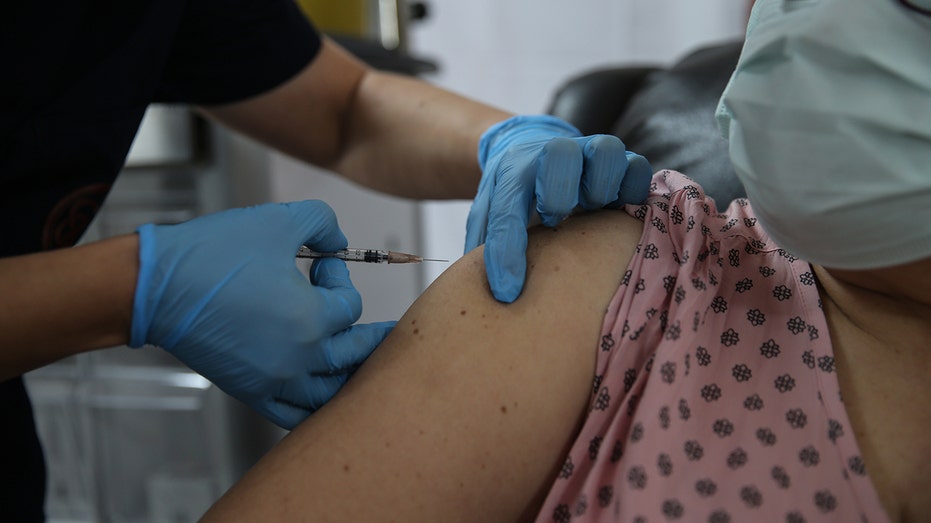
A health care worker injects a syringe of the phase 3 vaccine trial to a volunteer at the Ankara University Ibni Sina Hospital in Ankara, Turkey on Oct. 27, 2020. (Dogukan Keskinkilic/Anadolu Agency via Getty Images)
Days earlier, Moderna Inc. reported similarly strong preliminary results for its shot, which the biotech said was 94.5% effective in an early look.
The accumulation of positive data for the two shots suggests that drugmakers can develop vaccines capable of protecting against infections causing Covid-19 and its symptoms and that life could return to normal if sufficient numbers of people get inoculated.
Surveys show, however, that large percentages of people are hesitant to get the shots, partly out of concern the vaccines wouldn't be safe because their development was rushed.
PFIZER’S COVID-19 VACCINE PROVES 90% EFFECTIVE IN LATEST TRIALS
Drugmakers and health regulators have said they wouldn't allow a vaccine to go into use unless it is proven to work safely. If it shows to be without severe side effects in the final analysis, the Pfizer vaccine's safety data might help governments make the case for getting vaccinated.
Moderna, which is using the same kind of gene-based technology as Pfizer and BioNTech in its shot, is expected to report its safety data later this month.
Both shots work by delivering molecules, known as messenger RNA, that teach cells to make something resembling the spike protein that juts from the surface of the new coronavirus. Exposure to the protein preps a vaccinated person's immune system to fight off the virus.
In their late-stage, or Phase 3, trial, New York-based Pfizer and Germany's BioNTech directed that half the subjects receive the vaccine while the rest take a placebo.
Then the companies waited for enough volunteers to get exposed to the virus. They enrolled tens of thousands of subjects to increase the odds that some would develop Covid-19 with at least one symptom, though researchers needed only a fraction to assess using standard statistical methods whether the vaccine works safely.
The FDA required vaccine makers to monitor subjects for two months after their inoculation was completed because serious side effects usually crop up within roughly six weeks. The agency also wanted to see whether a vaccine was at least 50% effective.
For the final analysis of their Phase 3 trial results, the companies planned to wait for 164 study subjects to become infected and develop at least one symptom. Fifty-three of the sick subjects would need to have received the vaccine, with the rest getting the placebo, to be 52% effective, according to Pfizer's trial protocol.
By the time the final analysis occurred, researchers recorded several additional cases, bringing the total number of sickened subjects to 170. Researchers looked at how well the shots worked seven days after a study volunteer got a second dose.
PFIZER MAY APPLY FOR EMERGENCY USE OF COVID-19 VACCINE BY LATE NOVEMBER
The infected subjects included 10 severe cases of Covid-19, with nine in the placebo group and one in the vaccine group.
The vaccine was effective across different ages, races and ethnic groups, and it was more than 94% effective in adults over 65 years old, the companies said.
About 42% of the trial participants are from racial or ethnic minority groups, while 41% are ages 56 to 85, the companies said.
A committee of independent health experts analyzed the data from the trial, then reported the results to Pfizer and BioNTech. The companies released the data by press release and plan to publish the results in more detail later in a peer-reviewed medical journal.
Still unknown, as expected, is how long the protection provided by the shot lasts. To make such an assessment, Pfizer plans to monitor study subjects for two years.
PFIZER CEO SAYS CORONAVIRUS VACCINE COULD BE DISTRIBUTED TO AMERICANS BEFORE YEAR'S END
Also uncertain is whether the shots work safely in children, since the results are only for volunteers 18 years and older. Pfizer has expanded its trial to include children as young as 12.
The FDA is expected to take some time to consider requests for permission to distribute Covid-19 vaccines. One of the first steps will involve review by an outside committee of vaccine experts.
The FDA plans to conduct its review more quickly than it normally would because of the urgent need for the shots. If the agency finds the vaccines work safely, it will issue what it calls an authorization for emergency use, which the FDA invokes in pandemics.
During the current pandemic, the FDA has authorized for emergency use several drugs, including the antiviral remdesivir from Gilead Sciences Inc. and recently a Covid-19 antibody drug from Eli Lilly & Co.
Upon authorization, Pfizer plans to produce up to 50 million doses by the end of year, about half of which would be destined for the U.S. The supplies would be enough to inoculate only 12.5 million Americans because each person needs to take two doses three weeks apart.
PFIZER'S COVID-19 VACCINE: WHAT TO KNOW
Last summer, the U.S. agreed to pay Pfizer and BioNTech nearly $2 billion after it receives 100 million doses of their vaccine to provide to U.S. patients free of charge. The companies have struck similar supply agreements with other countries and are assembling a vast distribution network to begin shipping them, should regulators sign off.
The vaccine must be stored at minus 70 degrees Celsius, equivalent to minus 94 degrees Fahrenheit, which prompted Pfizer to create a special container to keep the shots cold during distribution and set up its own supply chain to ferry them around the globe.
The need for ultracold storage has also sent some health authorities and hospitals racing to find special freezers.
In the U.S., health officials are completing the plans for rolling out the vaccines. The Advisory Committee on Immunization Practices, a group of external medical experts that advises the Centers for Disease Control and Prevention, will vote on who should get initial doses. Health experts expect they will go to doctors and nurses treating Covid-19 patients.
A National Academy of Medicine panel recommended that next in line should be people whose health conditions put them at high risk of developing severe Covid-19, elderly people in nursing homes and people in prison. The panel said teachers and transportation workers should follow.
GET FOX BUSINESS ON THE GO BY CLICKING HERE
Health authorities expect that the general public could get vaccinated in the spring or summer.
Ronny Gal, a pharmaceutical analyst at Sanford C. Bernstein & Co., forecast in a research note Tuesday that vaccination in the U.S. would occur quickly and the country would achieve what is known as herd immunity, which would protect even the unvaccinated from the virus, by June.
Vaccine hesitancy would decline partly due to highly effective vaccines, Mr. Gal said.
Experimental vaccines from Johnson & Johnson and British drugmaker AstraZeneca PLC are also in Phase 3 testing, though results haven't come out yet. Novavax Inc. expects to begin late-stage testing of its vaccine in the U.S. and Mexico by the end of this month.
Vaccines developed in China and Russia are in use in certain countries.
CLICK HERE TO READ MORE ON FOX BUSINESS