What You Need to Know Before ObamaCare Open Enrollment
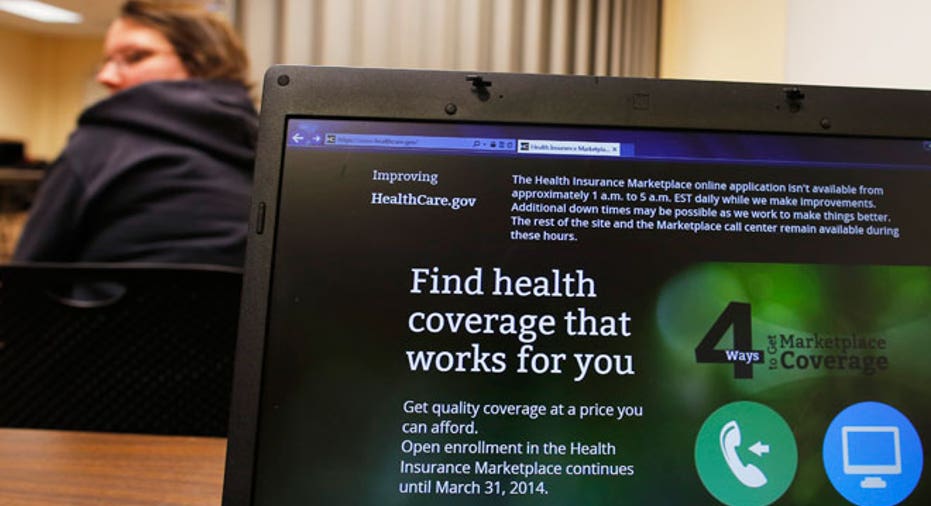
The second open enrollment for the Affordable Care Act begins this weekend. Eight million people signed up for private insurance in the Health Insurance Marketplace this year and current estimates suggest there are still about 32 million uninsured people in the U.S. The ACA improves access to affordable health coverage and the open enrollment period guarantees coverage of pre-existing conditions for all Americans.
I reached out to John Kelly, a nationally recognized health insurance exchange expert for tips on what we need to know about the ACA and open enrollment. Kelly, a principal business advisor at Edifecs, a health technology company, offered the following for my boomer readers:
Boomer: What changes if any have been made to the ACA for 2015? What is the open enrollment period for the Affordable Care Act and who does it apply to?
Kelly: The biggest change is the SHOP (Small Business Health Options Program) marketplace goes live November 15th in conjunction with the small business tax credits. The second biggest change is that most reviewers agree that the federal and state websites, though not perfect, are greatly improved over last year and there is little fear that they will crash and freeze with anticipated volume. Some minor changes include the Federal Exchange website offering many more options for filtering plans based upon special disease benefits and also much more flexible sorting capabilities to compare plans. Also, “passive enrollment” will allow people who enrolled through last year’s open enrollment to do nothing if they want their coverage to roll-over to 2015.
Overall, the Open Enrollment period to purchase healthcare coverage through the federal and state-run exchanges for coverage starting in 2015 begins on November 15, 2014-February 15, 2015. All American’s can sign up for health coverage through the exchanges including the young and healthy without employee-sponsored health benefits, the self-employed the unemployed and retirees. These segments, if gone uncovered, may have to pay a fee for being uninsured. Individuals who have access to qualifying employee sponsored plans will not be eligible for subsidies.
Those with Medicare don’t need to do anything – those individuals are covered and the ACA Open Enrollment period does not apply to Medicare choices or benefits. Those with qualifying retiree health benefits are considered covered under the healthcare law and won’t incur a fee.
Boomer: What is a health insurance exchange? Are there other types of health insurance available to individuals not on the exchange?
Kelly: Aside from making health insurance available to millions of Americans either denied access to affordable individual coverage or working without employer-sponsored benefits, a health insurance exchange is an online marketplace to purchase health benefits including medical, dental, and ancillary (life, vision, accident, etc.) coverage for individuals or families. The ACA specifically creates Federal and State based exchanges focused on healthcare benefits. If your state doesn’t operate its own “state-run” exchange, individuals looking to get covered would visit the federally-run exchange, HealthCare.gov. These marketplaces include ACA approved health plans and benefits packages. Individuals visit the exchanges like online shopping sites to search, compare competitive plans and eventually purchase their healthcare coverage. Purchased plans can be for family, as well as individual coverage.
There is an emerging group of health insurance offerings available to consumers outside of the public exchanges. It goes without saying that many will still get covered through employer-sponsored plans,
those eligible for Medicare and Medicaid can get covered through the government, and specialty programs like CHIPS are available for women and infants. Most private insurers also offer direct to consumer plans for individuals, families and those eligible for Medicare supplementary coverage. Alternatively, internet-based insurance brokers like ehealthinsurance (similar to Progressive where you can buy coverage for your car, home and other possessions) represent the convergence of both public and private exchange options. The Federal exchange has a contract with ehealthinsurance including a partnership to sell products from the Federal exchange and offer its calculator publicly for determining eligibility for subsidies and tax credits.
Boomers: How can baby boomers evaluate and pick the insurance plan that covers them best? Does a higher price tag mean better coverage?
Kelly: The first criteria enrollees should consider before evaluating insurance plans, is simply what they can afford. The available plans are must meet criteria for minimum coverage and do not vary greatly, so ultimately the first criterial should be budget.
The second phase in selecting care should be a detailed understanding of your needs. There is no need to compare preventative care costs as baseline plan must meet the care minimums for prevention and offer those benefits at no cost. You should ask yourself what is your lifestyle? Do you plan frequent visits? Do you have a chronic disease that requires intensive management? Do you see the doctor once a year for a physical? Do you want to partner with your doctor to extend beyond treatment and focus on wellness via wearables, nutritional counseling, exercise regimes or regular biofeedback sessions? These decisions will help determine the level of coverage you need from the perspective of your out of pocket costs.
Third, the boomer generation has become extremely savvy in their online shopping habits. This generation has the technological savvy to access online reviews from sites like National Committee for Quality Assurance (NCQA’s Private Health Insurance Plan Rankings 2013-2014 and NCQA’s Medicaid Health Insurance Plan Rankings 2013-2014), aarp.org and nerdwallet.com. These ranking sites for quality of care and service are invaluable in combination with research on each plan’s corporate website. Together these resources allow boomers to do a rigorous comparison of which plans offer simple administration, helpful information tools and most importantly, which plans offer the patients the best balance of risk against out of pocket costs for the services the consumer is most likely to need.
It’s a fine balancing act between selecting a monthly premium amount that can be afforded on a fixed income compared to how much care is needed throughout the year.
A higher price tag can sometimes mean more coverage but, it generally means lower out of pocket risk. In some cases it means more of one type of coverage, less of another. Overall, increased premiums have more to do with lowering your deductibles and individual cost sharing than with richness of benefit package. These decisions should be based on thinking about coverage that each individual hopefully will not need and use weighed against the risk of going without due to high out of pocket costs. A clear understanding of your risk profile should help inform these decisions. Ultimately, it’s all about downside risks, not upside gain – this is the basis of the entire exchange.
Boomer: My individual policy was canceled because it didn’t meet the requirements of the Affordable Care Act, according to a letter I got from my insurer. What options do I have?
Kelly: The exchange was designed to create a baseline of minimum coverage for all health plans looking to participate in the competitive market. The reason is, if plan doesn’t meet the minimum coverage requirements, someone could find out, at a very inopportune time, that what they thought they were paying for actually wasn’t available to them. The exchange is there to provide “credible care”- options available to a consumer when their plan didn’t provide meaningful protection against catastrophe – but as previously discussed, there are other options in the marketplace.
Ultimately, if your policy was cancelled, you can re-enroll on the exchange with a better coverage provider. But, before doing so, you should very seriously evaluate your criteria for selecting your plan. You were likely very lucky you did not need to use your policy.
Boomer: If your employer currently offers insurance, do you have to use that insurance, or do you have the option of selecting another plan?
Kelly: If you have employer offered coverage, you may be still able to change to a Marketplace plan. But you might not qualify for premium tax credits or other savings that make Marketplace insurance an affordable option. This will depend on two things:
- The type and cost of insurance your employer provides
- Your income and household size
However, if your employer-sponsored plan doesn’t meet the minimum levels of coverage stated in the ACA, then you would still be eligible for tax credits. Your employer has to meet minimum credible coverage standards.
Boomer: How do subsidies work?
Kelly: A subsidy (cost assistance) lowers the amount you spend on your monthly premium (via advanced premium tax credits) or reduces your out-of-pocket costs for things like copays, coinsurance, deductibles and out-of-pocket maximum (cost sharing reduction). Through the exchange your subsidy is factored upfront directly into your premium calculation. There are three types of subsidies available under law, tax credits, cost sharing reduction and Medicaid. For the eligible consumer under the exchange, the Federal government actually pays the insurer upfront for the care and this gets factored into the consumer’s monthly premium cost. However, at the end of the year, eligibility is recalculated and if there have been changes in income for example, a consumer might actually owe money back in taxes.
As an individual signs up on the insurance exchange and inputs their information, the system will automatically calculate your subsidies. There are calculators out there, such as this one through the Kaiser Family Foundation, that will provide premium estimates based on income, age and family size – these are great, free tools for getting a sense of what subsidies one is eligible for, including eligibility for Medicaid.
Boomers: Why might Boomers like the ACA?
Kelly: Boomers are the originators of the consumer economy. Ultimately the ACA, and the Exchange component in particular, is a mandate for the consumerization of healthcare purchasing. Boomers like choice and supplier competition; they like shopping online; they utilize the Internet to become educated consumers (Consumer Reports, Yelp, Angie’s list, etc.).
Boomers also feel squeezed as they age and lose access to good healthcare through job loss or job changes. A significant number of boomers are “healthcare tweeners,” too old to buy an affordable invincibles policy and too young to buy Medicare.
Many Boomers are also small business owners who feel a social obligation to provide healthcare options for employees but simply can’t afford the policies traditionally available to small businesses.
The ACA is designed to do three things:
- Create large pools of people among whom the costs of healthcare can be spread across lots of healthy and sick people. This is the foundation for affordability.
- Create a free market where insurers need to compete for individual consumer business, not for employer group purchases. Individuals are more inclined to purchase based upon value whereas employer groups place much more weigh cost.
- Place small and large businesses on near equal footing with regard to purchasing power in the healthcare marketplace.
For boomers, the ACA represents a curious combination of market based incentives for individual empowerment and a safety net to replace the social contract that they have seen erode between themselves and employers.



















