Why UnitedHealth Is the Only Healthcare Insurer To Own
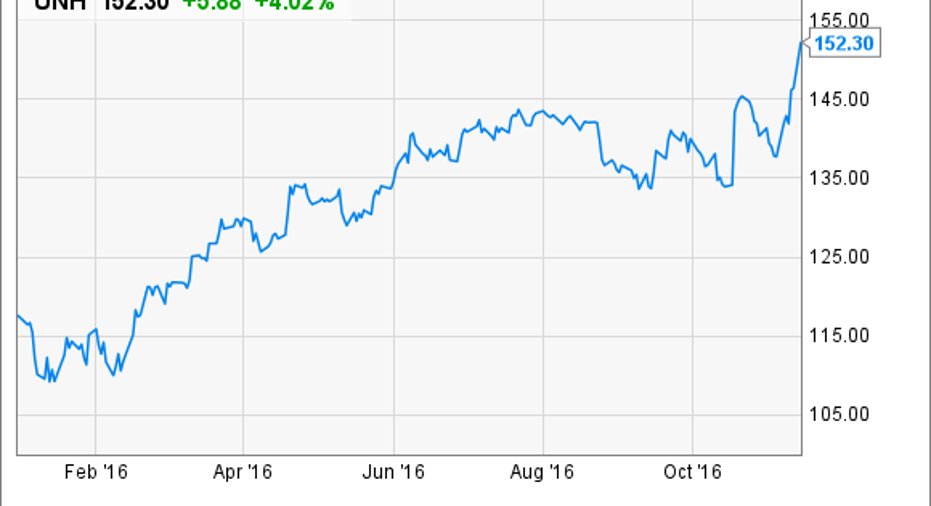
Image source: Getty Images.
Open enrollment forObamacare recentlykicked off, and the cost of the premiums will feel like a punch in the gut tomany Americans. On average, plans on the Affordable Care Act exchanges will cost a stunning 25% more than last year, and in some cases they will double.The increase won't just hit individuals and families hard; it's also bad news for investors in the majority of the nation's insurers.
Why? As premiums skyrocket, health insurance looks less worthwhile to healthy people, andhigh-utilization sick enrolleescreate dangerous financial losses for insurers.In fact,major insurers withheavy involvementin the ACA,such asAnthem (NYSE: ANTM), are taking it on the chin.Anthem reporteda bottom-line decline of 10.3% year over year in its third quarter.Thatstemmedfrom a9.4% rise in benefit expense, mostly due to ACA policies.
Meanwhile, Aetna (NYSE: AET) cited$430 million in lossesin insurance products since Obamacare began,withCEO Mark Bertolinipointing outthat the average price of ACA coverage is 10% to 15% below where it needs to be for insurers tobreak even, much less earn a dime.
With Trump victory, it's a whole new dayforinsurers
Adding to the turmoil,the new Trump administrationwillreshape the insurance marketplace.Some of Trump's proposed changes to the ACA,such asallowingcompetition across state lines,could further lower insurers' profits.But that's not thereal problem.The big issueis this: As we all know,themarket hates uncertainty, andthelevel of uncertaintyjust skyrocketed.
Insurerswho havespent years and millionstosell policies throughstate exchanges have no idea what their marketplace will look like in coming years.Millions of peopledepend on the ACA for coverage,so actual changes will take time. But meanwhile,insurers heavily involved inACAhave a much more risky outlook, and the market willreprice them downward -- sooner or later-- to reflect thatheightened risk.
Let's take alook at the firestorm now facing insurance stocks -- andwhy I believeUnitedHealth Group (NYSE: UNH), the insurerwith the leastexposuretoACA by far, is the onlyone to own.
Beer beats out insurance for young people
In addition topotentialmajor shifts in Obamacare,here's the mess thatfacesthe nation's insurers. With rates and deductibles rocketing upwardon ACA policies, fewerpeoplesee the plans as worthwhile.Consider this: The average American sees a physician only four times a year,with a retail cost of around$100 per visit,according to the National Center of Health Statistics.Whileplans vary greatly,a lower-cost ACA plan could nowrun$800 each month,and theindividual will have to pay out of pocket forthose doctor visits anyway, as deductibles can hit$10,000. IfACA coverage is subsidized, then the cost will be much lower -- perhaps only $800 per year -- but deductibles on lower-cost plans will still be sky-high. Meanwhile,subsidies also shift costs to taxpayers; the Congressional Budget Office estimates that this year's premium subsidies will reach$43 billion, or about $4,240 per subsidized enrollee.
Obamacare was supposed towork because the youngest, healthiest Americans wouldlower insurers' risk and thus lower the cost of coverage. But"even young people can do the math,"Aetna's CEOsaidrecently,claimingthat this group spendson"gas for the car, beer on Fridays and Saturdays" over health insurance.
Fears of an imbalanced risk pooland high medical costskeptUnitedHealtha minor player in the ACA -- a decision that nowlooks prescient.Noinsurer has proportionally less exposure thanthe nation's biggest, with only about 795,000ACA customers in total out of the 13 millionplans sold in 2016.Those policieswillsoon decline further,withUnitedHealthshrinkingACA coveragetothree states in 2017.
UnitedHealth's earnings blew it out of the park
One major reason ACA premiumssoaredis thatotherinsurers, such as Aetna and Humana (NYSE: HUM),arealso in the process of reducingor eliminating ACA coverage in many states.But UnitedHealth isso far ahead of the game that itraised the possibility of stronger profit growth in 2017,something no otherinsurer can boast. UnitedHealth alsouppedguidance on full-year 2016 earnings to $8 per share in its Q3 earnings,versus a previous view of $7.80-$7.95 per share. In addition,the company'sreportednet profit rose to $1.97 billion, or $2.03 per share, from $1.6 billion, or $1.65 per share, a year earlier.
Whilethis all signalsfurther stronggrowthahead for this stock,what impressed me the mostwasthatUnitedHealth'score insurance business beat outdrug benefits anddata analytics division Optumin revenue growth.Optum rosean impressive 9% to $21.1 billion,whilethe insurance business postedan almost torrid 13% growth rate.Optum has beena majorgrowth-driver for UnitedHealth for years,butthecore insurance business's growth adds another layer of security to this stock, because it indicates that the company is firing on all cylinders.
What about thedividend? UnitedHealth'spayout isa modest1.73%. But dividend growth counts more than current yield for many investors,and thedividend has leapt30% annually (on average) for the past fiveyears and is easily supported by apayout ratio below40%.
Meanwhile, worrieskeep piling up for other insurers
In addition tolosses intheir ACA segments,Anthem and Aetna facemajor merger issues.Last year, Anthem offered $54 billion to acquire Cigna (NYSE: CI), while Aetna offered$38 billion to take over Humana.Abrief euphoria droveshares oftheir acquisition targetsto new heights,but thosestocks droppedlike stoneswhenthe Department of Justice filed suit to block the mergers. Currently,both Humana and Cigna trade well belowtheiroffer prices,meaningthe market doesn't believethese deals will getdone.
Interestingly, Aetna has been paying hardball, telling the DOJit would probably be forced to withdraw from Obamacare altogether if the agency blocks its mergerover antitrust concerns. We "believe it is very likely that we would need to leave the public exchange business entirely and plan for additional business efficiencies should our deal ultimately be blocked,"CEO Mark Bertolini wrote in a July 5 letter.
Some have seen that as Aetna's payback to the Obama administration for blocking its merger. Aetna has now slashed its participation to just four states.
No crystal ball, but...
Lacking a crystal ball,there's no way to tellifObamacare willbe repealed, and many believe it won't be.That may be whythe insurers have moved up almost in lockstep with the election --it's hard for many to envision the U.S. without Obamacare,and the market isskeptical that the narrative has actually changed.
Butthat's ignoring the more immediateproblem: thedeteriorating risk pool andfinancial losses posed by the ACA. In addition, it's likely thatfears about the ACA'ssurvivalwill intensify as the Trump administration takes office, and if we start to see a slide,it could easilysnowball.
Investors willing to ride out the volatility in the other insurers will probably be fine in the long term,but it I'd recommend that you at least temper your expectations.Meanwhile,UnitedHealthisthe only insurer with thescale, thehistory, the diversification,and, most importantly, the lack of ACA sensitivity, to weather any storm that may come.
Forget the 2016 Election: 10 stocks we like better than UnitedHealth Group Donald Trump was just elected president, and volatility is up. But here's why you should ignore the election:
Investing geniuses Tom and David Gardner have spent a long time beating the market no matter who's in the White House. In fact, the newsletter they have run for over a decade, Motley Fool Stock Advisor, has tripled the market.*
David and Tom just revealed what they believe are the ten best stocks for investors to buy right now... and UnitedHealth Group wasn't one of them! That's right -- they think these 10 stocks are even better buys.
Click here to learn about these picks!
*Stock Advisor returns as of November 7, 2016
Cheryl Swanson has no position in any stocks mentioned. The Motley Fool recommends Anthem and UnitedHealth Group. Try any of our Foolish newsletter services free for 30 days. We Fools may not all hold the same opinions, but we all believe that considering a diverse range of insights makes us better investors. The Motley Fool has a disclosure policy.